HSCT for MS
HSCT (haematopoietic stem cell transplantation) is an intense chemotherapy treatment for MS. It aims to 'reset' the immune system by wiping it out and then regrowing it, using your stem cells.
Read our tips for talking about HSCT with your doctor or nurse
- What is HSCT
- Who can HSCT work for?
- How does HSCT treatment work?
- How well does HSCT work?
- What are the side effects of HSCT?
- HSCT, pregnancy, breastfeeding and contraception
- Getting HSCT and the MS Society
What is HSCT?
In MS the immune system mistakenly attacks the protective layer around nerves, called myelin. HSCT (haematopoietic stem cell transplantation) is a procedure that aims to reset the faulty immune system to stop this happening. It does this by partly or fully wiping out your immune system and then regrowing it using your stem cells.
Who can HSCT work for?
Research has shown that HSCT is most effective for people with MS who:
- have frequent relapses and MRI scans showing new or active lesions – these are signs of ‘active inflammation’
- are early on in their disease course
- don't have significant disability - measured by the EDSS (Expanded Disability Status Scale)
European guidelines are based on these research results. Most clinics use those guidelines to assess who can have HSCT.
You’re most likely to benefit if you have highly active relapsing MS and you're still having relapses despite taking disease modifying therapies (DMTs). That’s because HSCT targets the immune system causing the inflammation.
HSCT might also be able to slow down MS if you have progressive MS and still have active inflammation (either relapses or lesions on an MRI).
Find out more about who can get HSCT
Read the latest information about DMTs and coronavirus COVID-19
HSCT is unlikely to help if you have advanced progressive MS and you're no longer having relapses or signs of inflammation on an MRI. That’s because HSCT can’t repair the damage caused by this kind of MS.
Researchers are working hard to find effective treatments for people with progressive MS.
Read about our plan to stop MS
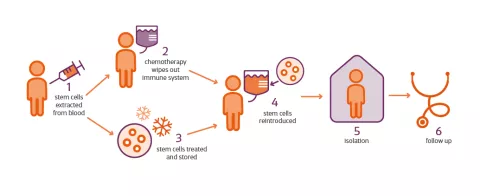
How does HSCT treatment work?
HSCT aims to 'reset' the immune system to stop it attacking the central nervous system. It uses chemotherapy to remove the harmful immune cells and then rebuilds the immune system using a type of stem cell found in your bone marrow. These are the haematopoietic stem cells.
The stem cells used in the treatment can produce all the different cells in your blood, including immune cells. But they can't regenerate damaged nerves or other parts of the brain and spinal cord.
Myeloablative and non-myeloablative HSCT
There’s more than one type of HSCT. They wipe out the immune system by different amounts to ‘reset’ it. One type is called ‘myeloablative’, which fully wipes out the immune system. Another is called ‘non-myeloablative’, which partly wipes it out. In the UK, non-myeloablative HSCT is used to treat MS.
How well does HSCT work?
DMTs can be put into three groups based on how well they control MS. HSCT is classed as 'high', the best of the three groups. This is based on how much it reduces relapses and slows down the rate at which people's disability gets worse.
Relapsing MS
Clinical trials have shown that HSCT is able to reduce relapses – mainly for people with relapsing MS. For some people their symptoms stabilise or get better, or their disability improves. But these improvements don’t always last.
A randomised control trial looked at 110 people with ‘very active’ relapsing MS. Half of them were treated with non-myeloablative HSCT and the other half with other DMTs. Non-myeloablative HSCT is the kind used to treat MS in the UK. The results showed:
- 99% of the people treated with HSCT had no relapses for 1 year. Only 1 person who had HSCT suffered a relapse. There were 39 relapses in people taking drug treatments
- 94% of people treated with HSCT didn’t see their disability get worse for 3 years (compared to 40% of those on drug treatments)
- EDSS scores (which measure disability) improved for the people treated with HSCT. For those on drug treatments, average EDSS scores got worse
Progressive MS
For progressive MS, we’ve seen some encouraging results for people treated early on in their condition, and where there’s still signs of inflammation (on an MRI scan, or in the shape of relapses). HSCT has been shown to slow down how fast MS gets worse in a few people who have early progressive MS.
Unfortunately, HSCT hasn’t worked as well for people with progressive MS who no longer show signs of inflammation and who have high levels of disability.
Read more about HSCT research studies
What are the side effects of HSCT?
Compared to other DMTs, HSCT has among the highest risk of side effects, especially serious ones.
HSCT side effects include:
- an increased long-term risk of developing infections
- an increased risk of developing cancer and autoimmune conditions, such as thyroiditis
- early menopause
- fertility problems
Chemotherapy - part of the HSCT procedure - has its own side effects too. These include an increased risk of bleeding and bruising, fatigue, loss of appetite and hair loss.
If someone has a high level of disability before the transplant, chemotherapy can also do more harm than good. Chemotherapy treatments can lead to your mobility getting worse and a worsening in how your nerves work.
The side effects of chemotherapy are more likely to be serious if you have the more intense type of HSCT – myeloablative, where the immune system is completely wiped out.
Some people have died as a result of HSCT. Since 2005, 1 person in about every 330 who have HSCT have died because of it. This risk can increase for people who are older, have a higher EDSS score, or have certain other conditions. A clinic offering HSCT should be able to explain your own risk, which will depend on lots of things, like your age and overall health.
HSCT and pregnancy, breastfeeding and contraception
Pregnancy
If you’re able to father a child or get pregnant, your medical team will give you advice before you have HSCT.
The chemotherapy drugs that you take with HSCT can harm an unborn baby and damage ovaries and testicles. This damage is often permanent, leaving you unable to have children (infertile). It can also cause an early menopause for women. Hormone replacement therapy (HRT) can help with menopause symptoms but it can’t stop the infertility.
Before you have HSCT, it’s possible to collect and freeze your eggs or sperm. You can then use them later to have children using procedures like IVF (in vitro fertilisation).
Your medical team will advise how soon after HSCT it’s safe to try to have a child.
Breastfeeding
High levels of chemotherapy drugs can get into breast milk. So breastfeeding must be avoided during HSCT. Your medical team will advise how soon after HSCT it’s safe to breastfeed.
Contraception
If you have periods, these can stop during chemotherapy, but you might still be producing eggs so you could still get pregnant.
Because chemotherapy drugs could harm an unborn baby, you should keep using reliable contraception. It takes about 6 to 12 months for periods to go back to normal. It’s important that you use contraception during this time. Your doctor should discuss all this with you.
Because chemotherapy damages sperm, men should get advice from their medical team about what type of contraception they should use.
Getting HSCT and the MS Society
We’re working alongside clinicians to help make sure people with MS can get treatments that are right for them at the right time. This includes HSCT for people that are eligible.
Read more about what we're doing for HSCT
StarMS clinical trial
Right now, the StarMS clinical trial is comparing HSCT with four other highly effective DMTs. The trial team are currently recruiting people with highly active relapsing MS.
Last full review:
We also update when we know about important changes.