Managing bladder problems
The first step to managing bladder problems is to talk to a specialist. Try not to worry about talking about bladder problems with your doctor or nurse. Health care professionals are used to talking about these issues and can offer help.
Virtually every area in the UK has a specialist continence service with at least one continence nurse (sometimes called an advisor). Continence nurses can provide information, for example, about products available, as well as confidential advice. You can 'self-refer' to most NHS Continence Advisory Services.
The Bladder and Bowel Community can give you details of your nearest service. You can also speak to a specialist nurse - calls are confidential.
Exercises for bladder problems
Training your pelvic floor muscles can help with some bladder issues. We worked with physiotherapist Rachel on a set of simple exercises for your pelvic floor muscles that you can try at home. There is an audio described version of this video.
Read more about pelvic floor muscle exercises below.
When your bladder doesn’t hold pee like it should
First line treatment
If things like changing how much you drink and what you eat don’t help, first line treatments are offered. These treatments are the ones most likely to work for most people. They include:
- bladder training
- drugs
- electrical stimulation
Bladder training
A continence nurse or bladder expert can help you train your bladder. You can learn to put off peeing for longer and longer periods. This stretches your bladder so that it holds more. You can also learn to only empty your bladder at set times (such as every two hours). This can ease the strong feeling of needing to pee.
Exercising your pelvic floor muscles is another way of getting your bladder to change how it behaves. Men and women can both do this. A continence nurse or physiotherapist can teach you how. It can stop your bladder leaking.
Drug treatments
Drugs can block the messages to your bladder that tell it to squeeze and empty. These drugs make it less irritable and overactive. You no longer feel you need the toilet all the time. There are seven of these ‘antimuscarinic’ drugs (sometimes called 'anti-cholinergic’ drugs). More than one in ten people who take them will get a dry mouth as a side effect.
Another drug called desmopressin causes your body to make less pee. This stops you from needing to get up in the night to use the toilet, letting you sleep better.
A drug called mirabegron (brand name Betmiga) relaxes the muscle in your bladder. This helps with urgency, frequency and incontinence.
Read more about these drugs in our booklet MS and your bladder.
Electrical nerve stimulation
Mild electrical signals can be sent to nerves that affect your bladder. An example is neuromuscular electrical stimulation.
For a set period you use a small battery-powered device to send electrical signals to nerves in your pelvic floor muscles that makes them squeeze. This way you learn to have more control over the muscles you use when you pee.
Second line treatments
If first line treatments don’t help your bladder to hold your pee like it should, then there are second line treatments. These include:
- botulinum toxin (Botox)
- electrical stimulation of your tibial nerve
Botox (botulinum toxin)
Botulinum toxin is better known by the brand name Botox. After giving you a local anaesthetic, a bladder doctor (urologist) injects it up to 30 times into the muscle in the wall of your bladder. This stops messages reaching your bladder that tell it to squeeze and empty. Your bladder will hold more, and you won't feel like going to the toilet so often.
The effects of Botox wear off eventually, so you need to keep having the injections every six to 12 months. Your GP can arrange a referral to a urologist for Botox treatment.
Botox can be very good at treating an overactive bladder. It's made a big difference to many people's lives. But usually it leaves you no longer able to empty your bladder. So you have to use a catheter each time you want to pee.
Stimulation of your tibial nerve
What if treatments like bladder training, drugs and Botox don’t work, or aren’t right for you? Then there's a treatment that might be available, depending on where you live: stimulation of your tibial nerve.
This nerve runs up your leg. Either a patch with an electrode in it is placed on the skin near this nerve or a needle is put into the skin above your ankle. A mild electrical current up is sent up the nerve.
This relaxes nerves in your lower back that control your bladder, helping to relax an overactive bladder. You have this done once a week for half an hour over three months.
Vibrating bladder stimulators
If you have problems with emptying or hesitancy, then holding a battery operated vibrating device or buzzer against your lower abdomen while going to the toilet may help. It’s thought to work by relaxing the sphincter muscle.
A continence adviser can advise you on using a bladder stimulator.
Pelvic floor exercises
Pelvic floor exercises can help with control by improving the ability to ‘hold on’.
You might have heard of women doing pelvic floor exercises after childbirth, but they can be done by men as well as women.
A physiotherapist or continence adviser can help you to learn how to exercise these muscles.
When your bladder doesn’t empty like it should
A test will show your if bladder isn’t emptying fully. When it doesn’t, pee is left in it. Bacteria grow in this, causing urinary tract infections. These can make your MS symptoms worse, and even trigger a relapse.
The usual treatment is for you to use catheters to empty your bladder properly. Some people find a vibrating device held near their bladder might also help it empty.
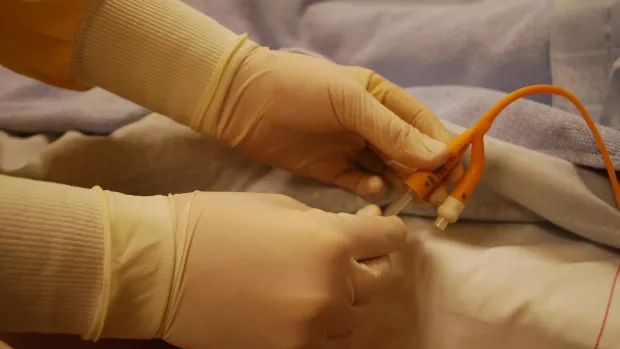
Catheters
A catheter is a small, flexible thin tube made from soft plastic, silicone or latex. You put it in your urethra. This is the pipe that takes pee from your bladder and out of your body. You push it in until it goes into your bladder. It’s not painful and many people with MS find it improves their quality of life a lot.
Intermittent self-catheterisation is a very good answer to a bladder that doesn't empty properly. This means every time you pee, you use a fresh catheter to empty your bladder.
A specialist nurse or continence adviser teaches you how to do this. They'll support you until you're confident enough to use a catheter.
Some people have a catheter that's inside their bladder all the time. These are indwelling catheters and are for people who can no longer walk. The catheter drains into a bag, usually attached to your leg with Velcro. When full, you empty the bag into the toilet. Or the catheter has a valve that lets you empty it straight into a toilet.
Indwelling catheters can go into your bladder through your urethra. They can also go into the bladder through a small hole made by a urologist in your belly. This is called a suprapubic catheter. Indwelling catheters need changing every three months by a nurse, with leg bags and valves changed every seven days.
Read Edith's experience of living with a permanent catheter in our community blog.
Vibrating bladder stimulators
Some people find that holding a battery-run device (often called a ‘buzzer’) over their pubic area can help their bladder empty. It vibrates, stimulating your bladder to relax and start emptying. For some people this can be an alternative to using catheters. You can bring this up with your continence nurse.
A continence nurse can also teach you ways of tapping your fingers or using your hand to put pressure on your lower belly. Both techniques can encourage your bladder to empty.
Managing day to day
What you eat and drink
It may seem illogical, but drinking more does tend to make bladder problems better. When you drink less, your urine becomes more concentrated. This can irritate your bladder, making it more likely to contract, and it can also make urinary tract infections (UTIs) more likely.
If you need to get used to drinking more, it is best to increase your intake gradually, for example on days when you are at home or when it is easy to get to a toilet.
Finding toilets when you're out
Carry our free 'I need some help' card. It explains you have MS and urgently need the toilet. Get it by calling 0300 500 8084 or email [email protected].
Find a public toilet at Toilet Map or download one of the public toilet apps.
Join the National (RADAR) Key Scheme. For a few pounds you get a key that lets you into over 9,000 locked accessible toilets in the UK.
If you need a public toilet bigger than standard accessible ones, or you need a hoist, check out Changing Places.
Contact your council to see if there’s a Community Toilets Scheme locally. It lets you use toilets in shops, restaurants and pubs without paying.
Continence products
ome people find using protective pads can help with managing bladder problems day-to-day. For men, penile sheaths can be helpful. These fit over the penis, and carry urine away through a tube to a small bag attached to the leg. Information is available from the Bladder and Bowel Community.
You can get products from your local continence service. Continence Product Advisor also offers unbiased advice and information on products like catheters, bags, pads, bed protection and special clothing.
A note on cranberry
Cranberry juice and cranberry extract tablets have both been studied in a number of research trials. But there is no conclusive evidence that they can help prevent or treat urinary tract infections for people with MS.