The journey of a drug
It takes a long time and lots of hard work to develop a new MS treatment. In 2019, ocrelizumab (brand name Ocrevus) became the first drug to be available for people with primary progressive MS on the NHS.
Join us as we journey through the years of research that led to this point.
The bright idea
All research starts with an idea.
It’s hard to pinpoint a single moment that sparked the journey of ocrelizumab. But a key event was the publication of results from a clinical trial of a different drug. These results suggested that a type of immune cell called a B cell could be important in MS.
Armed with this knowledge, scientists headed back to the lab to test their theory.
In the lab
There are a lot of tools that scientists use in the lab. Researchers around the world used different methods to find out more about the role of B cells in MS.
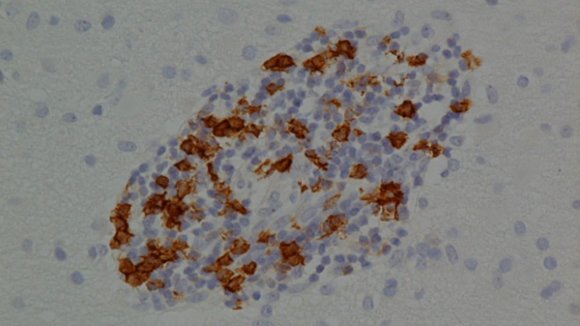
One way to better understand how cells function is to put them in a dish and examine them up close using a microscope.
Researchers also use human tissue. Brain and spinal cord tissue from the MS Society Tissue Bank was used to better understand the role of B cells in MS.
Cells and tissues can give us a lot of information about what’s going on at a biological level. But to fully understand what’s happening on a larger scale, researchers need to understand how a potential treatment works in animals with an MS-like condition.
In the UK all drugs must be tested in animals before they are tested in humans.
Read more about our research using animals
Clinical trials
If a treatment looks promising in the lab and is safe in animals, it can move into clinical trials to test the safety and benefits in humans.
Phase 1
Phase 1 trials test the treatment in a small group of people. Researchers check that it’s safe, measure the side effects and decide how it should be given.
Ocrelizumab was very similar to a drug that had already been through early testing so scientists already knew it was generally safe. It could therefore go straight into a Phase 2 trial.
Phase 2
If a treatment is successful in a Phase 1 trial, it goes into a Phase 2 trial. In this larger trial, researchers looked more closely at the safety and side effects compared to a placebo (dummy drug) in 220 people with relapsing MS.
The results of this trial found that ocrelizumab was safe and very few serious side effects were seen. So it continued to a Phase 3 trial.
Phase 3
Phase 3 trials compare the new treatment with the current standard treatment, or a placebo if another treatment isn’t available.
Ocrelizumab was tested for people with relapsing MS in two Phase 3 trials named OPERA 1 and 2. By running more than one trial, we can be sure we fully understand the effects of the treatment. The company manufacturing the drug also ran a Phase 3 trial for people with progressive MS called ORATORIO.
The results of these trials showed that ocrelizumab could reduce relapse rates and slow progression.
Making treatments available
Licensing
Once a treatment is shown to be safe and effective, it is submitted for a licence. In 2017, ocrelizumab was licensed by the European Medicines Agency (EMA) for people with relapsing MS and early primary progressive MS. A licensed treatment can be privately prescribed in the UK. But there is a final step.
Getting a treatment on the NHS
For a treatment to be made routinely available on the NHS it needs to be reviewed by the National Institute for Health and Care Excellence (NICE) in England and the Scottish Medicines Consortium (SMC) in Scotland. Authorities in Northern Ireland and Wales usually follow NICE recommendations. They look mainly at cost effectiveness.

In 2018, ocrelizumab was approved by NICE and the SMC as a treatment for relapsing MS. It was then approved as a treatment for early primary progressive MS in 2019.
Long term safety monitoring
Treatments are monitored for years even after they are licensed, to make sure we are keeping track of any side effects.
Speeding up clinical trials
Going from a scientific idea to a new treatment can take around 15 years. We want to reduce the time it takes to develop new treatments for people living with MS by speeding up clinical trials.
Read about the plans for our exciting new clinical trials platform